Why Athlete's Foot Is Not Just for Athletes
What is athlete's foot, and what are the symptoms?
You could say that athlete’s foot is an equal opportunity infection—it’s not just for athletes; anyone can get it. It is caused by the tinea pedis fungus,1 a type of dermatophyte, also responsible for jock itch and some kinds of ringworm. It usually takes up residence between the toes or elsewhere on the foot, and it is no fun. If you think you may have it, your best bet is to see a foot doctor right away, to get the most accurate diagnosis and learn how to treat the symptoms.
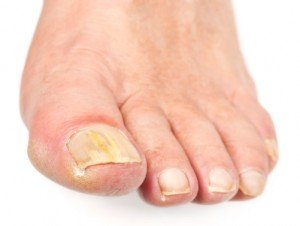
Characterized by extremely uncomfortable itching and burning, it can also cause skin to blister, crack, and peel, and is often accompanied by odor. Sometimes it shows up as redness and dryness or bumps on the soles of the feet. Toenails can be involved as well, looking ragged and discolored. Unfortunately, it is very good at spreading to other parts of the body, like the groin and the skin under your arms.
Who is prone to getting this fungal infection?
The most common victims of athlete’s foot are teen boys and young adult males. Athletes are among those who fall prey to this nasty fungus, but they are not the only targets. Women and girls can also develop it, as can anyone exposed to the right set of circumstances. It’s important to know what these right circumstances are—in other words, what to avoid.
There are two essential requirements for contracting athlete’s foot: 1: walking around barefoot where the fungus is found, and 2: giving that fungus a nice, warm, damp, sweaty, dark environment to grow in, like feet encased in tight shoes or sneakers.2

Another group commonly prone to the fungus includes people who wear plastic shoes. Plastic does not breathe the way leather and open shoes do, providing yet another comfy environment that allows fungus to grow, especially in a warm, damp climate.3
How to Avoid Athlete’s Foot
If there is just one overriding rule for avoiding athlete’s foot, it is this: keep your feet dry. Without moisture, the fungus can’t get a foothold (pun intended). Incorporate some daily habits into your life that will keep feet healthy and comfortable, including:
- Always dry your feet thoroughly after showering or swimming, especially between toes where moisture can lurk, inviting in bacteria and fungus.
- Wear shoes that fit well, allowing your toes to wiggle a bit. Tightly squeezed feet, especially when sweaty, are prone to developing athlete’s foot.
- Change to clean socks at least daily.
- Allow shoes to air out after wearing, and before storing away in a dark closet. This will help to reduce odor as well as discourage the growth of fungus.
- Wear open-toed shoes whenever possible, to give feet plenty of air and light.
- Wear flip-flops or other sandals of your own when walking around a locker room or public shower. This is prime territory for athlete’s foot, not because there are athletes, but because the environment has everything the fungus needs to become embedded and look for new victims.
- Clean bathroom and shower floors and tubs often to avoid the spread of germs at home.
- Avoid sharing towels, socks, or shoes, and try on shoes at the store wearing some kind of protection—this germ spreads by contact, and you might be sharing more than someone’s towel.
- Practice good hygiene by washing feet nightly before bed. The soles of the feet are often overlooked, when, in fact, they can play host to a multitude of germs and be the first point of contact for the athlete’s foot fungus.
How to Treat Athlete’s Foot
Once you have athlete’s foot, you need to take action right away to prevent its spread and to get rid of the uncomfortable blisters, itchy redness, and odors. There is a further risk, as you could develop a secondary bacterial infection that will spread further.2 Seeing a foot specialist is advisable to determine exactly what condition you have. The foot doctor can then prescribe the right treatment. Usually, an over-the-counter anti-fungal cream, spray, or powder will be effective within several weeks. If you follow instructions and symptoms don’t improve, you’ll want to go back to the doctor to see what additional treatment is needed, such as a prescription oral medication (pills).
Is It Gone Yet?
This fungus can be tough to kill. It may live with us even when we are feeling fine and unaware of its presence. It’s just when the environment encourages the fungus to grow out of control that we have a problem. It can easily recur once it gets started, so be sure to complete the doctor’s recommended course of treatment, even if your symptoms clear up before you finish your medication. Stopping too soon gives the fungus an opening to rebound and come back stronger than before.
Future Prevention
Besides the good hygiene habits mentioned above, and following “doctor’s orders,” there are a few additional steps to take that will prevent recurrence or the start of athlete’s foot in the first place, including:
- Switch from synthetic to cotton socks. Cotton breathes, pulling moisture away from your feet so they stay dryer. Synthetic fabrics trap moisture close to the skin, encouraging growth of bacteria or fungus.
- Use antifungal powder in athletic shoes or others that may retain the fungus.
- Going barefoot at home can help, giving your feet plenty of time to air out, as long as you keep floors and surfaces clean.1

If you are suffering foot discomfort or pain, and are unsure about the specific source, it is important to see a podiatrist or foot specialist. Sometimes, the emotional anguish and embarrassment that accompanies a foot problem is as significant as the medical problem itself. Your issue may go beyond the surface and include cosmetic challenges that lead you to hide your feet. As a result, following the advice to wear open-toed shoes and go barefoot is less appealing, and you may risk developing fungal or bacterial infections as a side effect of hiding your feet. If this sounds familiar, it is worth the time to schedule a consultation with an expert foot surgeon who can advise you on the possibilities for corrective surgery, if needed, or on less invasive forms of treatment.
Sources:
- http://www.webmd.com/skin-problems-and-treatments/athletes-foot-myths
- https://komonews.com/archive/athletes-foot-its-not-just-for-jocks
- Original Source (no longer available): http://www.goldenrule.com/health-wellness/what-causes-athletes-foot/