Different Arch Types: Associated Problems, Causes, and Treatment Options
Like the porridge in the Goldilocks story, foot arches should be not too high, not too low, but just right. Flat feet (fallen arches) and feet with very high arches (cavus foot) can both cause problems, and either extreme is considered an ailment of the midfoot.
As one flat-footed woman lamented in her blog post, high-heeled shoes are out of the question for her. Even a day out in flat shoes is so painful she makes fast friends with every bench or chair she comes across.

Having strong arches is important for physical stability, as the placement of your feet on the ground impacts the alignment of your entire body, from your ankles, to your knees, to your hips, back, shoulders, and neck. Your foot arches absorb stress, stabilize your body, and help you walk on uneven and sloping surfaces.
Below we’ll explore the anatomy of the foot, dii. We’ll also look at available treatment options to discuss with your foot specialist.
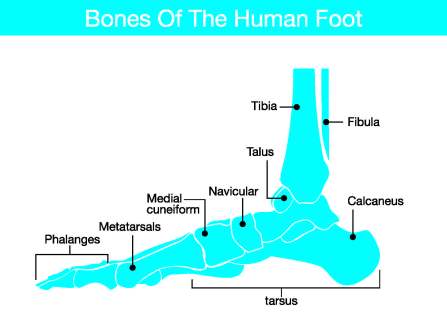
Anatomy of the Foot
Our feet are amazing structures. Made up of bones, joints, muscles, and soft tissues, our feet enable us to walk, run, jump, and pivot with precision. The foot has three segments: the forefoot, the midfoot, and the hindfoot.
- Forefoot: Made up of the five toes (phalanges) and the five longer bones (metatarsals).
- Midfoot: The collection of bones that form the arches of the feet; these bones include the cuneiform bones, the cuboid bone, and the navicular bone.
- Hindfoot: This segment makes up the heel and ankle, as well as the talus bone, which forms the ankle and supports the leg bones.
The muscles, tendons, and ligaments of the foot keep us balanced and allow for a wide range of motion.
Different Arch Types: Too High, Too Low, or Just Right
The arch of the foot generally falls into one of these four categories:
- Flat foot
- Medium (normal) arch
- High arch
- Very high arch (cavus foot)
The two extremes (flat foot and very high arch) tend to cause the problems. These are explored in more detail below.
Fallen Arches (Flat Feet)
Flat feet result from fallen or collapsed arches. The tendons and ligaments in your feet keep your arch stable; when they become weakened, flat feet can develop. In rare cases the development of flat feet starts in childhood; the foot’s arch never forms due to an abnormality that is sometimes hereditary.

More often, though, flat feet develop during adulthood due to excessive foot stress. Failure to properly treat an injury, such as an ankle sprain, or improper healing, can cause excessive strain that eventually leads to collapsed arches. Additional examples of excessive stress that can lead to collapsed arches include:
- Broken or dislocated bones in the feet or ankle.
- Nerve problems.
- Wearing shoes without proper arch support.
- Stretched or torn tendons.
- Damage to or inflammation of the posterior tibial tendon, which connects your lower leg to the middle of your foot arch via the ankle.
- Rheumatoid arthritis and other inflammatory conditions.
- Weakened muscles in the foot and ankle from weight gain or aging.
A common problem associated with flat feet is over-pronation, which means the foot rolls inward too much. This can lead to a host of problems, including plantar fasciitis, heel pain syndrome, bunions, tendonitis, and others. If you have flat feet, it may take years for problems to emerge. Eventually you may experience foot pain and notice increased strain on your feet and calves from over-pronation.
Diagnosing Flat Foot
How do you know if you have flat feet? Here’s an easy way to find out:
First, consider whether you frequently experience foot or ankle pain, feel pain or discomfort when walking or standing for long periods of time, have strained posture, or have feet that turn in at the ankle. If you answered yes to any of these questions, you may have flat feet.
To find out for sure, wet your feet and stand on a surface that shows your full foot imprints (a brown paper bag or a concrete sidewalk both work well). The image below shows what the typical imprint looks like for people with different arch types. Normal arches will reveal a slight curve on the inner part of the foot, while a flat foot shows nearly the entire outline of the foot.
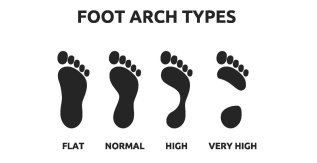
Non-Surgical Treatments for Flat Feet
Your foot doctor will recommend several non-surgical options to manage pain and discomfort from flat feet. They may include:
- Wearing orthotic shoe inserts or footwear.
- Resting and icing feet at home when you have pain.
- Taking non-steroidal ant-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen.
- Avoiding activities that put excessive stress on your feet, such as running on hard surfaces.
- Avoiding high-impact sports.
Risk factors that can worsen flat feet include obesity, diabetes, and high blood pressure.
Surgery for Flat Feet
In cases of severe foot damage, your foot specialist may recommend surgery. Procedures to correct fallen arches include:
- Arthrodesis, which involves fusing the foot or ankle bones together.
- Osteotomy, in which the foot surgeon cuts or changes the shape of the foot bones.
- Lateral column lengthening, in which the surgeon grafts bone to your foot to increase the arch.
- Tendon transfer, which involves taking tendon tissue from another part of your body and adding it to your foot to create more “pull” of the tendons, resulting in a better formed arch.
Now let’s look at the counter to flat feet—very high arches.
Very High Arch (Cavus Foot)
Cavus foot is a condition in which one or both feet have very high arches. The condition places excessive weight on the ball and heel of the foot, which can lead to a variety of problems, including hammertoes, claw toes, pronounced calluses on the side, ball, and heel of the foot, instability when standing, and pain when standing, walking, or running.

Cavus foot can develop at any age. It is often caused by neurological conditions like cerebral palsy and muscular dystrophy, as well as other medical conditions, such as spina bifida or stroke. Cavus foot can also be caused by an inherent structural abnormality of the foot.
Supination is a common problem with cavus foot and causes the foot to roll outward (the opposite of pronation). Supination can cause the knee and pelvis to tilt back; it can also prevent the foot from properly absorbing shock, all of which can lead to pain in the feet, knees, hips, back, shoulder, and neck.
Diagnosing Cavus Foot
Your foot doctor will review your family history and examine your feet, looking for signs of very high arch, including those mentioned above (calluses, hammertoes, and claw toes). Your doctor may also test your foot and muscle strength, observe your walking pattern, and order x-rays of your feet and spine.
Non-Surgical Treatment for Cavus Foot
Your doctor will likely recommend the following non-surgical options to treat cavus foot initially:
- Orthotic devices: Custom inserts that fit into your shoes to help stabilize your foot and provide cushioning.
- Bracing: A brace made of semi-flexible material to help stabilize your foot and ankle.
- Orthotic shoes: Custom-made shoes with high tops that support the ankle and wider bottoms to improve stability.
Surgery for Cavus Foot
Surgery is generally the last option to treat cavus foot, but it may be necessary in severe cases. The various surgeries for cavus foot are all intended to provide more even weight distribution on the inside and outside edges the foot. Surgical procedures include:
Soft-tissue surgery, which can include procedures to partially or completely release (loosen) the plantar fascia, lengthen part of the calf muscle or Achilles tendon, or surgically transfer tendons or muscles that are causing too much pull.
- Dorsiflexion osteotomy of the first metatarsal to flatten out the arch.
- Bone surgery to correct the deformity of the foot; this can include bone cuts (osteotomies) or fusion (arthrodesis) procedures.
- Toe surgery to correct claw toes, which are a common problem with very high arch. Toe surgery may also involve fusion or removal of part of the toe bones, or tendon surgery.
Any surgery comes with risks, but for many it’s necessary to relieve the often significant pain, discomfort, and gait abnormalities associated with foot arch problems. Surgery can also improve the appearance of your feet, making you less reluctant to go barefoot. Your foot surgeon will work closely with you to determine the best treatment option for you.